WHAT IS POLYCYSTIC OVARY SYNDROME?
Polycystic ovary syndrome (PCOS) is a hormonal disorder frequent among women of reproductive age. Women with polycystic ovary syndrome (PCOS) might have infrequent or prolonged menstrual periods or excess male hormone (androgen) levels. The ovaries might develop numerous small collections of fluid (follicles) and fail to regularly release eggs.
The exact cause of polycystic ovary syndrome (PCOS) is not known. Early diagnosis and treatment along with weight loss might lower the risk of long-term complications like type 2 diabetes and heart disease.

POLYCYSTIC OVARY SYNDROME SYMPTOMS
Signs and symptoms of polycystic ovary syndrome (PCOS) generally develop around the time of the first menstrual period during puberty. At times polycystic ovary syndrome (PCOS) develops later, for instance, in response to substantial weight gain.
Signs and symptoms of polycystic ovary syndrome (PCOS) differ. A diagnosis of polycystic ovary syndrome (PCOS) is made when you experience at least two of these signs:
- Irregular periods – Infrequent, irregular, or prolonged menstrual cycles are the most frequent sign of polycystic ovary syndrome (PCOS). For instance, you might have fewer than 9 periods a year, more than 35 days between periods, and abnormally heavy periods.
- Excess androgen – Increased levels of male hormones might result in physical signs, like excess facial and body hair (hirsutism), and at times serious acne and male-pattern baldness.
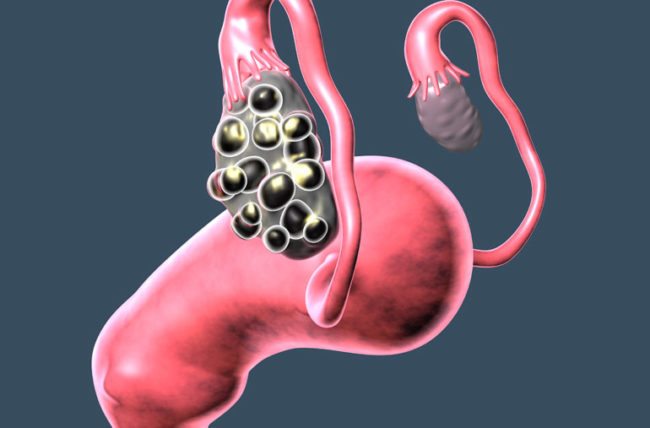
- Polycystic ovaries – Your ovaries may be enlarged and contain follicles that encircle the eggs. Therefore, the ovaries may fail to function regularly.
Polycystic ovary syndrome (PCOS) signs and symptoms are generally more severe if you are overweight.
WHEN SHOULD YOU SEE A DOCTOR?
See your doctor or primary care physician if you have issues with your menstrual periods, if you are experiencing infertility or if you have signs of excess androgen-like worsening hirsutism, acne, and male-pattern baldness.
POLYCYSTIC OVARY SYNDROME CAUSES
The precise cause of polycystic ovary syndrome (PCOS) is unknown. The following factors may play an important role:
- Excess insulin – Insulin is the hormone produced in the pancreas that permits cells to use sugar, your body’s main energy supply. If your cells become resistant to the action of insulin, then your blood sugar levels could rise and your body may produce more insulin. Excess insulin may raise androgen production, causing difficulty with ovulation.
- Low-grade inflammation – This term is used to describe white blood cell’s production of substances to combat infection. Research has indicated that women with polycystic ovary syndrome (PCOS) have a type of low-grade swelling that stimulates polycystic ovaries to produce androgens, which could lead to heart and blood vessel problems.
- Heredity – Research suggests that specific genes might be linked to polycystic ovary syndrome (PCOS).
- Excess androgen – The ovaries produce abnormally elevated levels of androgen, resulting in hirsutism and acne.
POLYCYSTIC OVARY SYNDROME COMPLICATIONS
Complications of polycystic ovary syndrome (PCOS) could include:
- Infertility
- Gestational diabetes or pregnancy-induced high blood pressure
- Miscarriage or premature birth
- Non-alcoholic steatohepatitis is a serious liver swelling caused by fat accumulation in the liver
- Metabolic syndrome — a cluster of conditions including high blood pressure, high blood sugar, and abnormal cholesterol or triglyceride levels that significantly raise your risk of cardiovascular disease
- Type 2 diabetes or prediabetes
- Sleep apnea
- Depression, anxiety, and eating disorders
- Abnormal uterine bleeding
- Cancer of the uterine lining (endometrial cancer)
Obesity is associated with polycystic ovary syndrome (PCOS) and could worsen complications of the disorder.
POLYCYSTIC OVARY SYNDROME DIAGNOSIS
There is no test to definitively diagnose polycystic ovary syndrome (PCOS). Your doctor or primary care physician is likely to start with a discussion of your medical history, including your menstrual periods and weight changes. A physical examination will include checking for signs of extra hair growth, insulin resistance, and acne.
Your doctor or primary care physician may then recommend:
- A pelvic examination – The doctor or primary care physician visually and manually examine your reproductive organs for masses, growths, or other deformities.
- Blood tests – Your blood might be analyzed to measure hormone levels. This testing could exclude possible causes of menstrual abnormalities or androgen excess that mimics polycystic ovary syndrome (PCOS). You may have additional blood testing to measure glucose tolerance and fasting cholesterol and triglyceride levels.
- An ultrasound – Your doctor or primary care physician checks the appearance of your ovaries and the thickness of the lining of your uterus. A wand-type device (transducer) is placed in your vagina (transvaginal ultrasound). The transducer emits sound waves that are translated into pictures on a computer screen.
If you have a diagnosis of polycystic ovary syndrome (PCOS), your doctor or primary care physician may recommend additional tests for complications. Those tests could include:
- Periodic checks of blood pressure, glucose tolerance, cholesterol, and triglyceride levels
- Screening for depression and anxiety
- Screening for obstructive sleep apnea
POLYCYSTIC OVARY SYNDROME TREATMENT
Polycystic ovary syndrome (PCOS) treatment focuses on managing your individual concerns, like infertility, hirsutism, acne, or obesity. Specific treatment may involve lifestyle changes or medication.

POLYCYSTIC OVARY SYNDROME CAUSES
Lifestyle changes
Your doctor or primary care physician might recommend weight loss through a low-calorie diet combined with moderate exercise activities. Even a modest reduction in your weight, for instance, losing five percent of your body weight may improve your condition. Losing weight might also increase the effectiveness of medications your doctor or primary care physician recommends for polycystic ovary syndrome (PCOS) and could help with infertility.
Medications
To regulate your menstrual cycle, your doctor or primary care physician may recommend:
- Combination birth control pills – Pills that contain estrogen and progestin lessen androgen production and regulate estrogen. Regulating your hormones could lower your risk of endometrial cancer and correct abnormal bleeding, excess hair growth, and acne. Instead of pills, you may use a skin patch or vaginal ring that contains a combination of estrogen and progestin.
- Progestin therapy – Taking progestin for ten to fourteen days every one to two months could regulate your periods and protect against endometrial cancer. Progestin therapy does not improve androgen levels and would not prevent pregnancy. The progestin-only mini pill or progestin-containing intrauterine device is a better choice if you also wish to circumvent pregnancy.
To help you ovulate, your doctor or primary care physician may recommend:
- Clomiphene – This oral anti-estrogen medication is taken at the time of the first part of your menstrual cycle.
- Letrozole (Femara) – This breast cancer treatment could work to stimulate the ovaries.
- Metformin – This oral medication for type 2 diabetes improves insulin resistance and reduces insulin levels. If you do not become pregnant using clomiphene, your doctor or primary care physician may recommend adding metformin. If you have prediabetes, metformin could also slow the progression to type 2 diabetes and help with weight loss.
- Gonadotropins – These hormone medications are administered by injection.

To reduce excessive hair growth, your doctor or primary care physician may recommend:
- Birth control pills – These pills decrease androgen production that could cause excessive hair growth.
- Spironolactone (Aldactone) – This medication obstructs the effects of androgen on the skin. Spironolactone could cause birth defects, so effective contraception is required while taking this medication. It is not recommended if you are pregnant or planning to become pregnant.
- Eflornithine (Vaniqa) – This cream could slow facial hair growth in women.
- Electrolysis – A small needle is inserted into each hair follicle. The needle emits a pulse of electric current to damage and ultimately destroy the follicle. You may require multiple treatments.
If you or anyone you know is suffering from polycystic ovary syndrome (PCOS), our expert providers at Zenith Injury Relief & Wellness Clinic will take care of your health and help you recover.
Call 972-210-0033 to schedule your appointment, and begin living your life pain-free.
