Plantar fasciitis is one of the most common reasons to visit a podiatrist. In everyday life, your plantar fascia ligaments experience a lot of wear and tear. These ligaments are not able to bear too much pressure causing damage or tear the ligaments.
Plantar fasciitis is a degenerative condition. This affects the thick band of tissue known as fascia. The tissue is present at the bottom of your foot that runs from your heel to your toes.
Doctors thought that the bony growths called heel spurs are the reason for this pain. But, it was discovered that heel spurs are the result and not the cause of plantar fasciitis. The plantar fascia ligament becomes inflamed causing heel pain and stiffness.
People suffering from plantar fasciitis cause stabbing pain. The pain usually occurs with your first steps in the morning. The pain subsides as you get up and move. But, it might return after standing for a long duration or when you stand up after sitting.
Plantar fasciitis occurs in runners, overweight people, and people wearing inadequate footwear support.

WHAT CAUSES PLANTAR FASCIITIS?
You are at a high risk of developing plantar fasciitis if:
- You are between the age of 40 and 70 and are active, then you are at the risk of developing plantar fasciitis. It is usually more common in women than men, especially in pregnant women. Pregnant women often experience bouts of plantar fasciitis, during the later stage of pregnancy.
- You are overweight or obese you’re at a greater risk of developing plantar fasciitis. Extra weight that you gained suddenly increases pressure on your plantar fascia ligaments.
- You’re a long-distance runner due to increasing pressure for a long duration.
- You have a very active job that involves being on your feet for a long duration.
- You have structural foot problems, such as very high arches or very flat feet.
- Tightness in Achilles tendons connecting calf muscles to your heels causes pain in the plantar fascia.
- You have an unusual walking pattern or foot position.
- You often wear high-heeled shoes in daily life or for a long duration.
- You wear worn-out shoes with thin soles.
- You change your activity level like working out to lose weight.
- You exercise and do not stretch your calves.
Plantar fasciitis is not the result of heel spurs but vice versa heel spurs are the result of plantar fasciitis.
There are various other causes of plantar fasciitis, including:
- The strain on the Achilles tendon
- Flat feet
- High arches
- Changes in walking or running patterns
- Using shoes with poor cushioning
- Long periods of standing or walking
- Running on soft surfaces
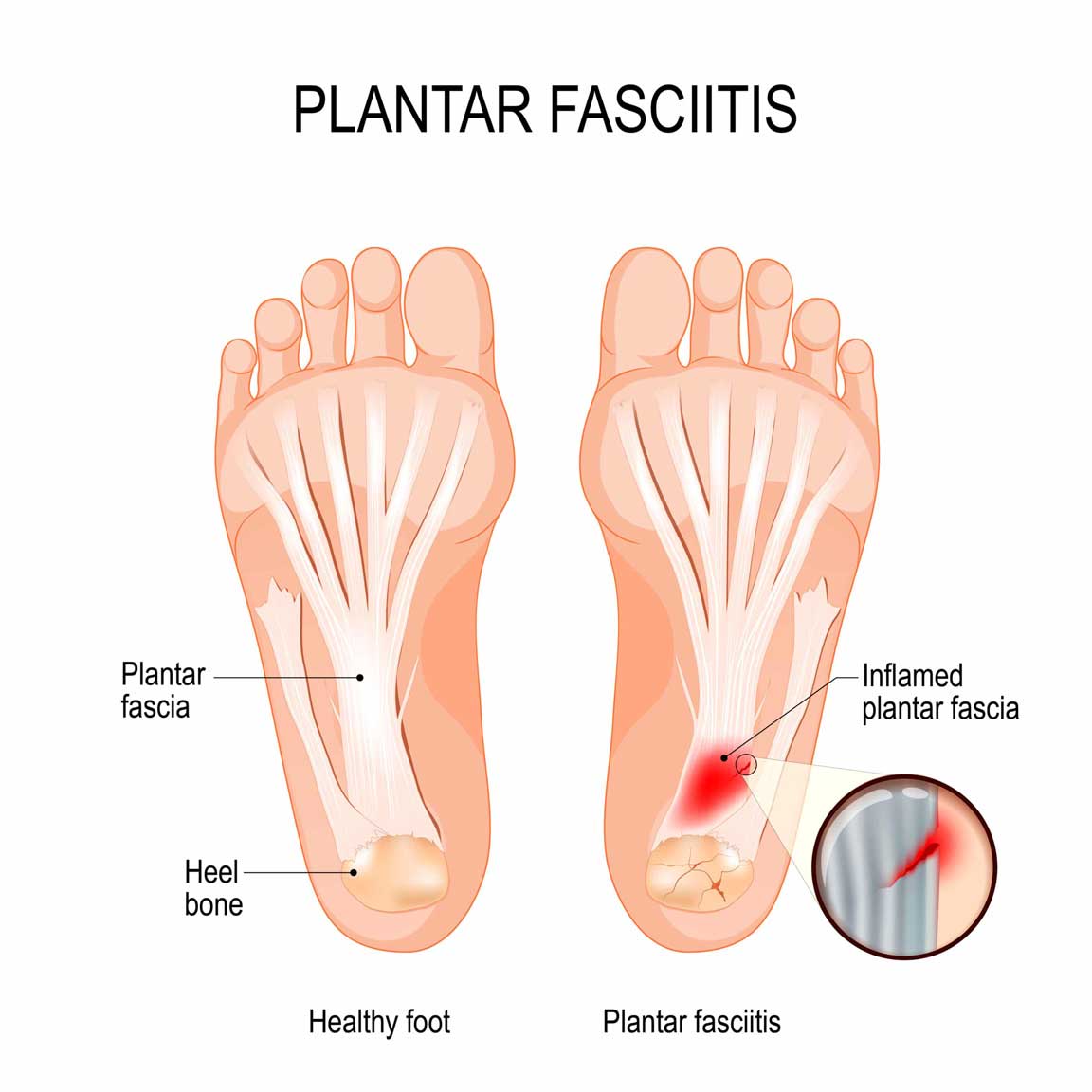
WHAT ARE THE SYMPTOMS OF PLANTAR FASCIITIS?
If you are suffering from plantar fasciitis you experience pain at the bottom of the heel or sometimes even at the bottom midfoot area. The pain is usually dull and stabbing in nature in patients with plantar fasciitis.
The pain develops gradually over some time. You usually might experience pain in one foot but it may affect both feet. Your first steps in the morning are usually the worst with plantar fasciitis. You may also experience intense heel pain when you get out of bed or after long periods of sitting.
You would feel that the pain reduces when you move around as the affected muscle warms up. But, this does not imply that your problem is going away. It has been observed that plantar fasciitis gets worse over time. Sometimes, even walking can help reduce the immediate pain from standing, but it might eventually flare up again with prolonged periods of standing or walking.
The symptoms of plantar fasciitis include:
- Pain on the bottom of the heel, or near the affected area.
- Increased pain after exercise but not during the exercise.
- Pain in the arch of the foot.
- Pain worsening in the morning or when you stand after sitting for a long time.
- Swelling in the heel.
- Pain continued for months.
A tight Achilles tendon, which connects the calf muscles to your heel. About 80% of people report this symptom.
HOW TO DIAGNOSE PLANTAR FASCIITIS?
The doctor would initially perform a physical examination to check for inflammation, tenderness, and the exact location of the pain in the foot.
Your podiatrist would check the strength of your foot muscles and the health of your nerves by checking the:
- Reflexes
- Muscle tone
- Sense of touch and sight
- Coordination
- Balance
Looking at the symptoms they would sometimes want you to have imaging tests to make sure something else isn’t causing your problem. These tests include:
- An X-ray to rule out bone fractures or arthritis.
- An MRI to look for fractures.

HOW TO TREAT PLANTAR FASCIITIS?
Plantar fasciitis can be usually treated by home treatment remedies such as:
- Resting the affected foot,
- Icing the area of pain,
- Using braces or orthotics, and
- Medications such as anti-inflammatory drugs and painkillers.
If the above home treatments do not ease the pain, the podiatrist would recommend an injection of a corticosteroid directly into the damaged section of the ligament. Corticosteroids can also be applied to the skin of your heel or the arch of your foot. Further, painless electrical current is applied to let the steroid pass through your skin and into the muscle.
Physical therapy provides most relief in pain of plantar fasciitis. This includes exercises to stretch your plantar fascia and Achilles tendons, which strengthens your lower leg muscles, helping to stabilize your walk and lessen the workload on your plantar fascia. Massage with essential oils such as lavender oil, lemongrass oil, eucalyptus oil or rose oil along with carrier oil (like coconut oil) also helps to reduce pain and inflammation caused by plantar fasciitis.
Diet also plays a significant role in preventing plantar fasciitis to develop again. Supplements such as vitamin C, zinc, glucosamine, bromelain and fish oil help with tissue repair and healing.
Extracorporeal shock wave therapy also helps in treating plantar fasciitis. The sound waves bombarded at the affected area stimulate healing within the ligament.
In severe cases, where home treatments do not provide relief for more than 6 to 12 months, surgery is the only option. The surgeon would partially detach the plantar fascia from the bone to reduce tension. This would weaken the arch of the foot, and full function may be lost. Surgery might also result in chronic pain and nerve damage. Due to these implications, surgery is considered only after trying other treatment options.
OUTLOOK
Mostly you would not need surgery to relieve pain from plantar fasciitis. The condition can be easily improved with physical therapy, home treatments, and medical treatments. Experts at Zenith Injury Relief & Wellness Clinic focus on providing quick relief with minimally-invasive treatment methods.
If you or anyone you know is suffering from heel pain, our expert providers at Zenith Injury Relief & Wellness Clinic will take care of your health and help you recover.
Call us on 972-210-0033 to book an appointment with our specialists, and begin living your life pain-free.
